Metabolic adaptation
Weight loss via caloric restriction can trigger a persistent physiologic response called metabolic adaptation2,3
The Tug-of-War in the Body
Dr. Lofton explains how metabolic adaptation creates a battle between weight loss and regain.

Video length: 1:30
Which hormones are affected by metabolic adaptation?
Metabolic adaptation may result in increased signals for energy intake (increase in the hunger hormone [ie, ghrelin] and decrease in satiety hormones [eg, GLP-1, PYY, CCK, amylin]).3*
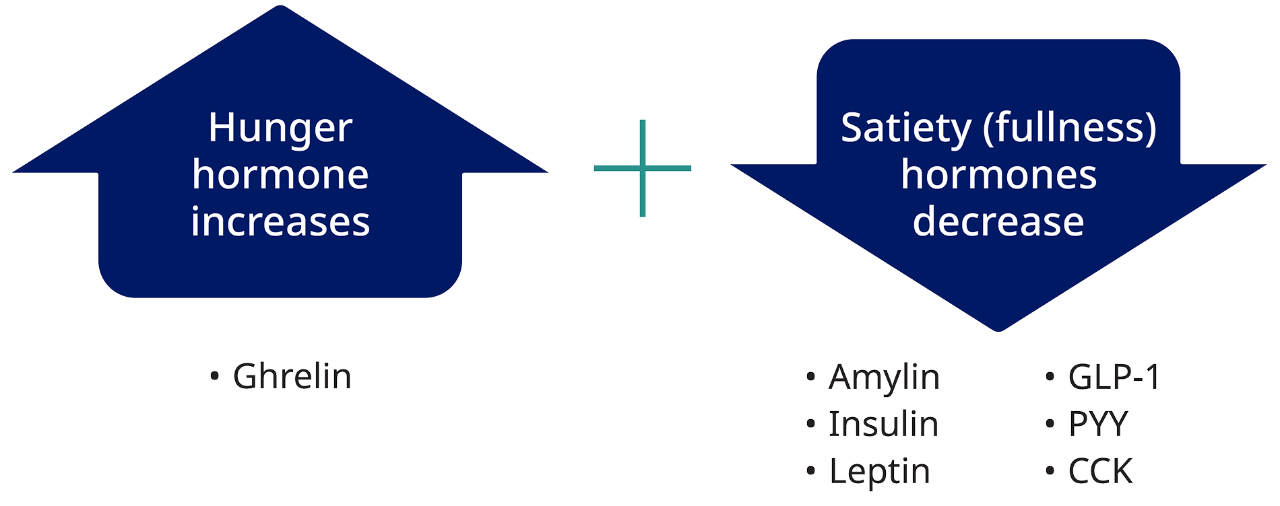
*Study design
Study enrolled 50 adults with overweight or obesity, without diabetes, in a 10-week weight-loss program, with a very-low-energy diet prescribed. The circulating levels of leptin, ghrelin, peptide YY, gastric inhibitory polypeptide, GLP-1, amylin, pancreatic polypeptide, cholecystokinin, insulin, and subjective ratings of appetite were examined at baseline (before weight loss), at 10 weeks (after program completion), and at 62 weeks.3

“Obesity is a legitimate, complex, relapsing, chronic disease at the root of so many metabolic complications. We need to identify and treat it just like we’ve been trained to treat any other chronic disease.”4
Sandra Sobel, MD
Endocrinologist, Board-Certified in Obesity and Lifestyle Medicine
The brain plays a critical role in appetite regulation
For people with obesity trying to lose weight and maintain it, managing hunger can be a major challenge.5-10
A team of hormones from the body, including GLP-1, signal to the brain, affecting food intake9,10
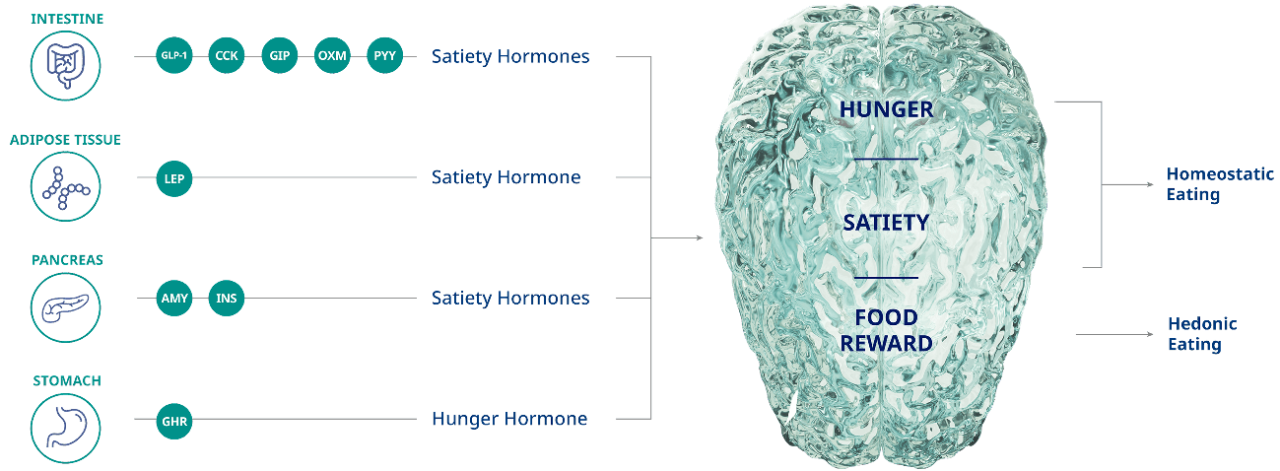
AMY, amylin; CCK, cholecystokinin; GHR, ghrelin; GIP, glucose-dependent insulinotropic polypeptide; GLP-1, glucagon-like peptide-1; INS, insulin; LEP, leptin; OXM, oxyntomodulin; PYY, peptide YY.
After weight loss due to caloric restriction, metabolic adaptation can lead to decreases in resting metabolic rate and lower energy expenditure2
Most of the energy expenditure comes from resting metabolic rate2
- In the beginning of a calorie-restricted diet, there is a reduction in energy intake that occurs more rapidly than the reduction of energy expenditure, creating an acute energy deficit that induces weight loss11
- Metabolic adaptation occurs when the decline in energy expenditure is beyond what would be expected relative to changes in body mass or composition11
- Circulating hormones (including leptin, thyroid hormones, and insulin) may mediate changes in metabolic activity11
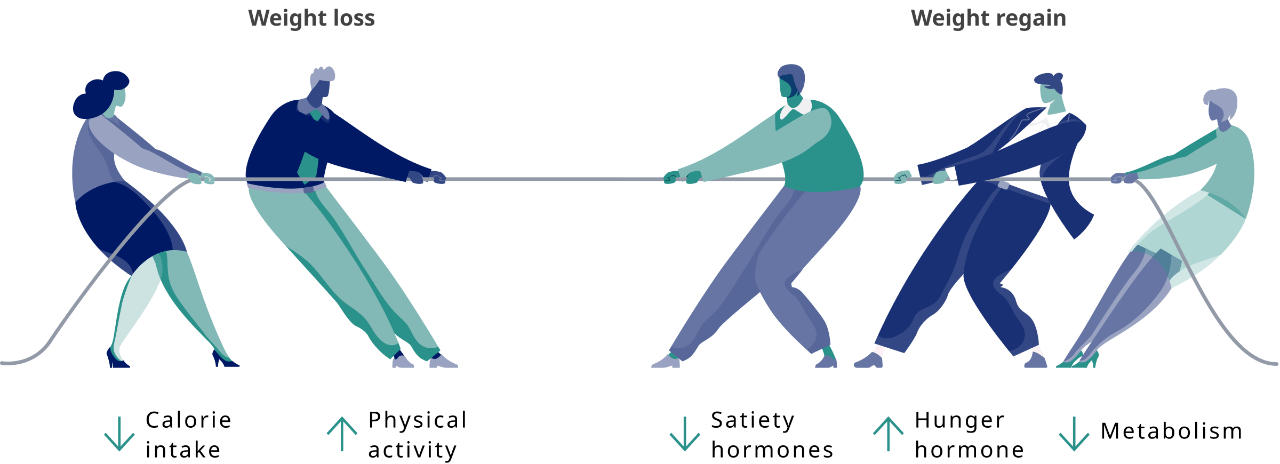
Why patients with obesity often regain lost weight
Less than half of people with obesity reported having maintained weight loss for more than 1 year.12† This may be because weight loss triggers multiple physiological processes that defend baseline body weight. A study showed that the mechanisms contributing to weight regain can persist for at least 1 year.3‡
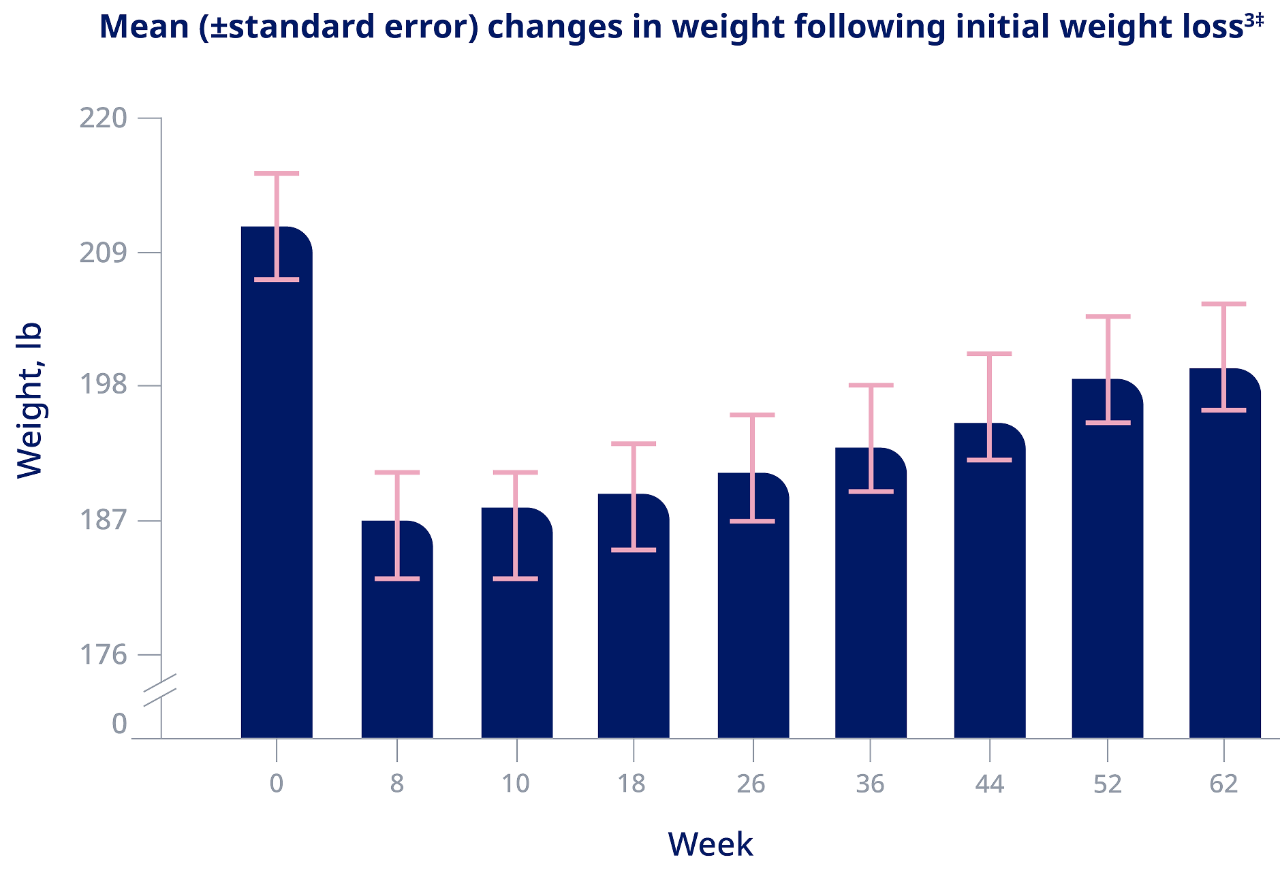
†
Results from quantitative surveys in a study of over 3,000 adult patients with a mean BMI of ≥37 kg/m² based on self-reported height and weight. Forty-four percent of people with obesity who reported a weight loss of at least 10% from their maximum weight during the previous 3 years maintained that weight loss for more than 1 year.12
‡
Study design
The study enrolled 50 patients with overweight or obesity, with a BMI between 27 kg/m² and 40 kg/m², who were prescribed a very-low-energy diet (500-550 kcal/day) for 8 weeks. Participants who lost 10% or more of their initial body weight by the end of week 10 were then gradually reintroduced to ordinary foods and received individual counseling from a dietitian for 1 year with the aim of weight maintenance. They were also encouraged to engage in 30 minutes of moderately intense physical activity on most days of the week. Circulating levels of appetite-regulating hormones were measured at baseline (week 0) and at weeks 10 and 62, which were compared with baseline levels.3
1. Zhu B, Gostoli S, Benasi G, et al. The role of psychological well-being in weight loss: new insights from a comprehensive lifestyle intervention. Int J Clin Health Psychol. 2022;22(1):100279.
2. Lam YY, Ravussin E. Analysis of energy metabolism in humans: a review of methodologies. Mol Metab. 2016;5(11):1057-1071.
3. Sumithran P, Prendergast LA, Delbridge E, et al. Long-term persistence of hormonal adaptations to weight loss. N Eng J Med. 2011;365(17):1597-1604.
4. Garvey WT, Mechanick JI, Brett EM, et al; Reviewers of the AACE/ACE Obesity Clinical Practice Guidelines. American Association of Clinical Endocrinologists and American College of Endocrinology comprehensive clinical practice guidelines for medical care of patients with obesity. Endocr Pract. 2016;22(suppl 3):1-203.
5. Yu JH, Kim MS. Molecular mechanisms of appetite regulation. Diab Metab J. 2012;36(6):391-398.
6. Austin J, Marks D. Hormonal regulators of appetite. Int J Pediatr Endocrinol. 2009;2009:141753.
7. Guyenet SJ, Schwartz MW. Regulation of food intake, energy balance, and body fat mass: implications for the pathogenesis and treatment of obesity. J Clin Endoc Metab. 2012;97(3):745-755.
8. Farr OM, Li CR, Mantzoros CS. Central nervous system regulation of eating: insights from human brain imaging. Metab Clin Exp. 2016;65:699-713.
9. Cassidy RM, Tong Q. Hunger and satiety gauge reward sensitivity. Front Endocrinol (Lausanne). 2017;8:104.
10. Druce MR, Small CJ, Bloom SR. Minireview: gut peptides regulating satiety. Endocrinology. 2004;145(6):2660-2665.
11. Most J, Redman LM. Impact of calorie restriction on energy metabolism in humans. Exp Gerontol. 2020;133:110875.
12. Kaplan LM, Golden A, Jinnett K, et al. Perceptions of barriers to effective obesity care: results from the National ACTION Study. Obesity (Silver Spring). 2018;26(1):61-69.




